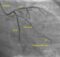
Coronary artery perforation during PCI
Coronary artery perforation during PCI
Coronary artery perforation is an important but rare complication of percutaneous coronary intervention. Perforations can be caused by guide wires, angioplasty balloons or rotablator burr. It is a potentially life threatening complication depending on the severity and immediate management options available.
Ellis classification of coronary artery perforations
Ellis classification is based on angiographic appearance of the perforation.1
Grade I: Extraluminal crater without extravasation
Grade II: Pericardial or myocardial blushing
Grade III: Perforations of one or more millimeter diameter with contrast streaming or spilling
Predictors of coronary perforation during PCI
Perforations are more likely to occur with rotablator than conventional PCI. It is more likely in advanced age and females. Grade III perforations with the worst prognosis are more likely to occur with complex lesions and chronic total occlusions.2 But even smaller perforations can have unexpected problems and hence close monitoring for at least 24 hours is mandatory.
Management of coronary artery perforations
Immediate treatment options include prolonged balloon inflations and implantation of covered stents apart from reversal of heparin. Cardiac tamponade should be aspirated and auto transfused if needed. Surgical repair and coil embolisation are other options. Small perforations in insignificant vessels can also be managed by applying negative suction in a wedged microcatheter so as to produce vessel collapse and obliteration.
References
- Ellis SG et al. Increased coronary perforation in the new device era. Incidence, classification, management, and outcome. Circulation. 1994 Dec;90(6):2725-30.
- Al-Lamee R et al. Incidence, predictors, management, immediate and long-term outcomes following grade III coronary perforation. JACC Cardiovasc Interv. 2011;4:87-95.