ECG Challenge – Discussion
Salient findings and diagnosis?
ECG Challenge – Discussion
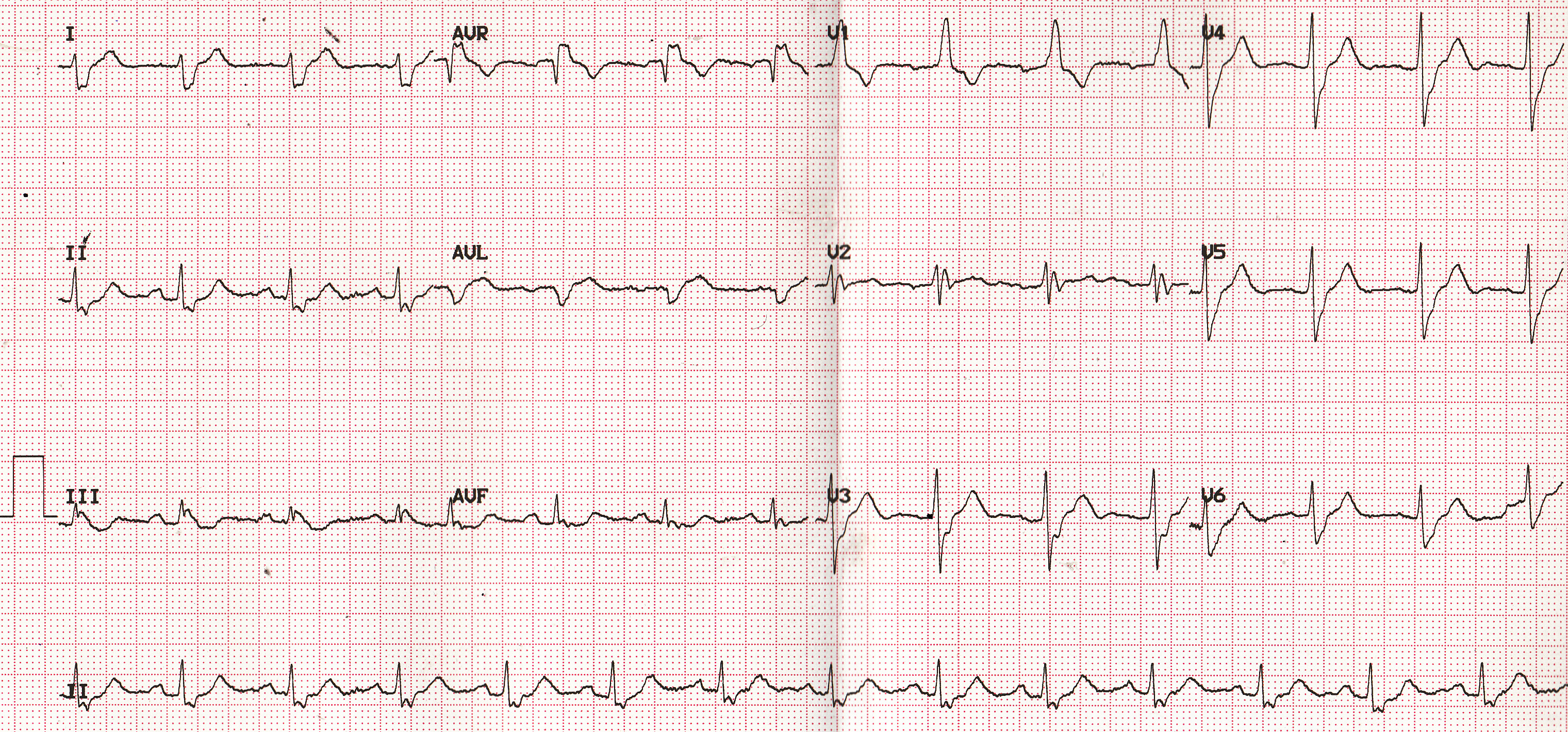
ECG shows sinus rhythm with heart rate around 83/min. QRS width is around 160 ms. rS pattern in lead I and QS in aVL would mean right axis deviation, in this case due to right posterior hemiblock (LPHB). Notched R in V1 and rsr’s’ in V2 with slurred S in lead I, V5, V6 suggests right bundle branch block (RBBB). Together these will constitute a bifascicular block. Bifascicular block is diagnosed when any two of the three fascicles of His-Purkinje system are involved. But usually it means right bundle branch block with either left anterior (commoner) or the left posterior hemiblock. Even though left bundle itself constitutes two fascicles, left bundle branch block is seldom called bifascicular block.
Left posterior hemiblock is diagnosed based on the abnormal right axis deviation. Slurred S wave in RBBB causes some difficulty in assessing right axis deviation. In general, QRS axis during the first 80 ms of the QRS can be considered to make this assessment.
PR interval is 200 ms, the upper limit of normal. P wave is wide in leads II and III suggesting left atrial overload. But the negative component of P wave in V1 is not very prominent. If PR interval prolongs further it will become trifascicular block, which is quite near a complete heart block. Electrophysiological study with measurement of HV interval may have a role in predicting which of the patients with bifascicular block are likely to progress to complete heart block [1].
Reference
- Israel CW. Syncope and bifascicular block: who needs a pacemaker? Rev Esp Cardiol. 2010 Apr;63(4):385-6.


