Echocardiographic profile in pulmonary hypertension
Echocardiographic profile in pulmonary hypertension
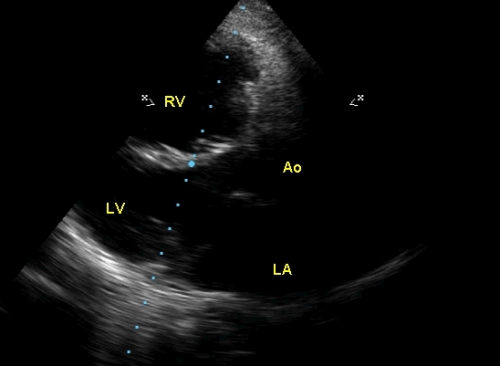
Echocardiogram in parasternal long axis view shows a dilated right ventricle, with a measurement of 4.2 cm in this view. Normally only a much smaller portion of the right ventricle is visible in this view. A better view to assess the right ventricle would be the apical four chamber view. Ao: aorta; LA: left atrium; RV: right ventricle; LV: left ventricle
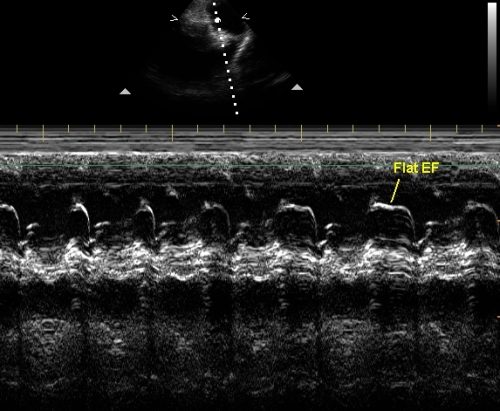
M-mode echocardiogram of the pulmonary valve level showing features of pulmonary hypertension – a flat EF slope and shallow A wave. The A wave in pulmonary valve M-mode echocardiogram becomes shallow in pulmonary hypertension and prominent in pulmonary stenosis. M-mode echocardiogram to assess the pulmonary valve was routine in the era when Doppler echo was not available. But now this modality is seldom used as the right ventricular systolic pressures can be measured much more accurately from the tricuspid regurgitation jet by Doppler echocardiography using the Bernoulli equation. PV: pulmonary valve
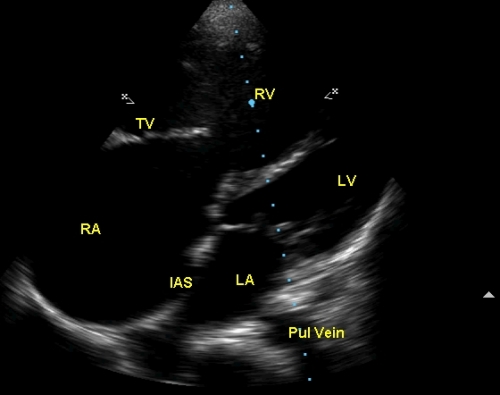
A modified apical four chamber view in pulmonary hypertension showing the dilated right ventricle and right atrium. The inter atrial septum is seen to be convex, bulging towards the left atrium due to the elevated pressures in the right atrium. An echo drop out is seen in the region of fossa ovalis due to the thinness of the stretched septum in that region. RA: right atrium; RV: right ventricle; LV: left ventricle; LA: left atrium; IAS: inter atrial septum; Pul vein: pulmonary vein
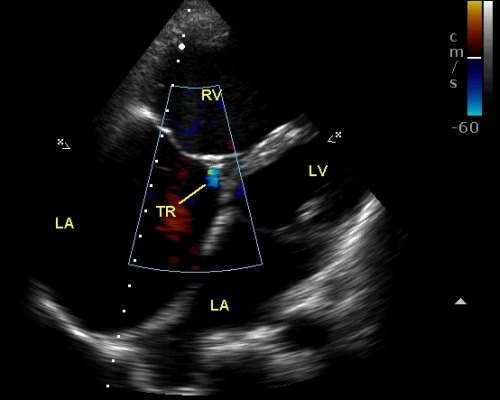
Color flow mapping in the modified apical four chamber view shows trivial tricuspid regurgitation (TR) as a tiny mosaic coloured bluish jet from the right ventricle to the right atrium, across the closed tricuspid valve. Doppler cursor can be aligned to this jet only with difficulty and a good envelope may not be obtained. Hence the estimation of the right ventricular systolic pressure from the TR jet will be difficult in this case. Multiple tilted views may be imaged in an attempt to get better TR signals.
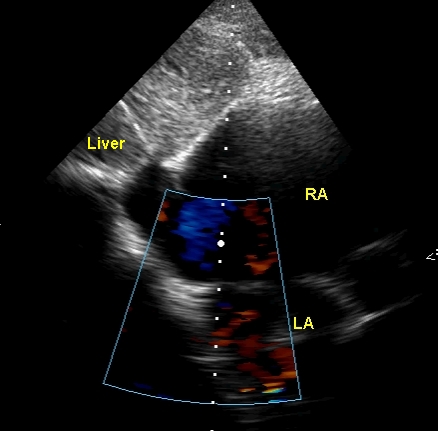
Subcostal view with color flow mapping (colour Doppler) shows that the there is no flow across the interatrial septum although there was a suspicion of an echo drop out. But there may not be any significant flow across the interatrial septum even with an atrial septal defect (ASD) if the right atrial pressures are elevated and equal to that of the left atrium and the compliance of right ventricle is reduced due to hypertrophy. In such situations a transesophageal echo may be able to confirm the presence of an ASD. In some cases, cardiac catheterisation and angiography may be required in addition.
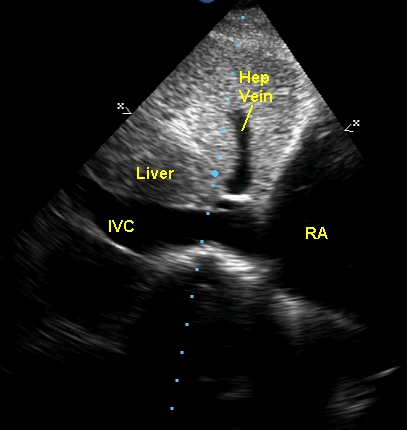
Subcostal view imaging the inferior vena cava (IVC), liver and hepatic veins (Hep vein). The IVC was dilated and showed little collapse with inspiration (IVC plethora), indicating high venous pressure. Normally the respiratory variation in IVC size is more than 50%.