Role of Valsalva maneuver in cardiology
Role of Valsalva maneuver in cardiology
The initial description of Valsalva maneuver was published by Antonio Maria Valsalva in 1704. It was forced expiratory effort against the closed glottis, nose and mouth, lasting for a few seconds. The maneuver was employed with the aim of expelling foreign bodies or exudates from the middle ear [1]. Even today otolaryngologists use variations of the maneuver very often. Edward Weber in 1851 detailed the cardiovascular changes associated with maneuver, making it useful for diagnostic purpose. Hence some authors prefer to call it as Valsalva-Weber maneuver [2].
The classical four phases of Valsalva maneuver and its hemodynamic effects were described by Hamilton WF et al in 1936. In 1947 Rushmer made the assessment objective by expiratory straining against the mercury column of a sphygmomanometer. Later this was changed to an aneroid manometer for better convenience [1].
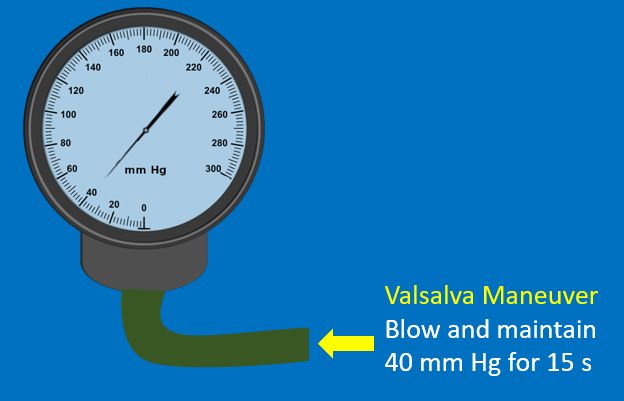
The subject is asked to take a full inspiration and blow against the resistance of a mouth piece connected to an aneroid manometer to maintain a pressure of 30 – 40 mm Hg for 15 – 20 seconds. It is then released and normal respiration resumed without gasping. Venous return decreases during the strain phase and reduces blood pressure which triggers baroreceptor mediated increase in heart rate. After cessation of straining, there is abrupt reversal resulting in overshoot of arterial pressure, which is known as Valsalva overshoot. This leads to baroreceptor mediated bradycardia. Finally the hemodynamic changes return to basal levels [1]. While feeling the pulse during a Valsalva maneuver, it is easy to appreciate the bradycardia during phase IV.
The classical four phases of Valsalva maneuver can be better documented by invasive intra arterial pressure recording along with electrocardiographic monitoring. Phase I is associated with transient rise in arterial pressure and bradycardia at the beginning of strain due to increase in intrathoracic pressure. Phase II is the maintenance of straining with progressive decrease in arterial pressure and reflex tachycardia. Phase III is release of strain with a transient dip in arterial pressure with tachycardia. Phase IV is the phase of post straining arterial pressure overshoot associated with bradycardia.
Valsalva maneuver is used in clinical cardiology for the ascertaining origin of various cardiac murmurs. Typical example is differentiating the murmurs of aortic stenosis and hypertrophic obstructive cardiomyopathy. Murmur of aortic stenosis decreases due to the reduced left ventricular end diastolic volume. But a reduced end diastolic volume worsens the obstruction in hypertrophic obstructive cardiomyopathy and accentuates the murmur. Therapeutic use of Valsalva murmur in the termination of supraventricular tachycardia is well known. Sometimes it is useful in elucidating the mechanism of supraventricular tachycardia.
Valsalva maneuver is used in the assessment of cardiac autonomic function. Valsalva ratio is the ratio of maximal tachycardia to the maximal bradycardia induced by the maneuver [3]. RR intervals from an ECG monitor can be used for this purpose. Valsalva delay is the time for the maximum RR interval variation from phase III to IV.
Square wave response is the absence of the typical declining slope of the arterial pressure in the strain phase [4]. This is because the preload of an overloaded left ventricle does not decrease significantly. Arterial pressure increases with strain and returns to normal on release of strain.
References
- Junqueira LF Jr. Teaching cardiac autonomic function dynamics employing the Valsalva (Valsalva-Weber) maneuver. Adv Physiol Educ. 2008 Mar;32(1):100-6.
- Derbes VJ, Kerr A Jr. Valsalva’s maneuver and Weber’s experiment. N Engl J Med. 1955 Nov 10;253(19):822-3.
- Levin AB. A simple test of cardiac function based upon the heart rate changes induced by the Valsalva maneuver. Am J Cardiol. 1966 Jul;18(1):90-9.
- Kapur NK, Jumean M, Halin N, Kiernan MS, DeNofrio D, Pham DT. Ventricular square-wave response: case illustrating the role of invasive hemodynamics in the management of continuous-flow left ventricular assist device dysfunction. Circ Heart Fail. 2015 May;8(3):652-4.