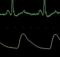
Slow ventricular tachycardia
Slow ventricular tachycardia
Slow ventricular tachycardia is ventricular tachycardia with rate less than typical. Hence it can be missed especially in those on pacemakers who already have a wide QRS rhythm. In one case report, the person presented with features of liver failure secondary to heart failure [1]. Pacemaker analysis showed atrioventricular dissociation, markedly higher ventricular rate compared to atrial rate with absence of ventricular stimulation. It did not respond to eight biphasic shocks of 200 Joules. It was also unresponsive to amiodarone and lignocaine.
An earlier report of two cases highlighted the fact that a high index of suspicion for slow ventricular tachycardia is needed in patients on antiarrhythmic drugs [2]. They mentioned that ventricular tachycardia may be mistaken for supraventricular tachycardia with aberrant conduction, with the possibility of incorrect diagnosis in as many as 30% of cases. Slow ventricular tachycardia is thought to be more common in those with implantable cardioverter defibrillator than in general population. Antiarrhythmic agents like amiodarone and beta blockers may lower the rate of any breakthrough ventricular tachycardia to rates as low as 100-120 beats/min.
An international multicenter prospective randomized study assessed the incidence and clinical relevance of slow ventricular tachycardia in those with implantable cardioverter defibrillator [3]. The study had 374 patients without prior history of slow VT with rate less than 148 beats/min, implanted with dual chamber ICD. Three zone detection configuration was with slow VT zone 101 to 148 beats/min, conventional VT zone with rate above 148 beats/min and a ventricular fibrillation zone. Treatment group had 183 patients with therapy activated in the slow VT zone and the monitoring group had 191 patients with no therapy in slow VT zone. During a 11 month follow up, 181 slow VTs were documented in 54 patients in the monitoring group. In the treatment group, 250 slow VTs were documented in 60 patients. 245 episodes were treated with antitachycardia pacing with a success rate of 89.8%. 5 episodes decelerated spontaneously. Shock was delivered in two patients with ATP failure. In those patients in whom shock delivery in slow VT zone was not programmed, some episodes terminated spontaneously while some progressed to conventional VT zone and got treated. Quality of life score was not different between the groups. Overall, the study reported 30.4% incidence of slow VT in ICD recipients without a prior history of symptomatic or ECG documented slow VT.
Another study evaluated the clinical relevance of slow VT in symptomatic heart failure patients with primary prophylactic ICD indication, with or without concomitant cardiac resynchronization therapy [4]. Devices were programmed to an additional monitor zone for slow VTs at 130-186 beats/min. 200 patients were followed up for a mean period of 509 days. 137 were in New York Heart Association functional class III, 75 patients were on CRT and 124 had ischemic cardiomyopathy. Only 12 patients had slow VT though there were 473 episodes of VT in 36 patients and 131 episodes of ventricular fibrillation in 30 patients. No patient with slow VT had syncope, palpitation or decompensation leading to hospitalization.
References
- Wannhoff A, Nusshag C, Stremmel W, Merle U. Slow ventricular tachycardia presenting with acute liver failure. SAGE Open Med Case Rep. 2017 Jul 12;5:2050313X17718100. doi: 10.1177/2050313X17718100. PMID: 28835821; PMCID: PMC5528920.
- Leitz N, Khawaja Z, Been M. Slow ventricular tachycardia. BMJ. 2008 Jul 3;337:a424. doi: 10.1136/bmj.39489.687894.DE. PMID: 18599467.
- Sadoul N, Mletzko R, Anselme F, Bowes R, Schöls W, Kouakam C, Casteigneau G, Luise R, Iscolo N, Aliot E; Slow VT Study Group. Incidence and clinical relevance of slow ventricular tachycardia in implantable cardioverter-defibrillator recipients: an international multicenter prospective study. Circulation. 2005 Aug 16;112(7):946-53. doi: 10.1161/CIRCULATIONAHA.105.533513. PMID: 16103252.
- Lüsebrink U, Duncker D, Hess M, Heinrichs I, Gardiwal A, Oswald H, König T, Klein G. Clinical relevance of slow ventricular tachycardia in heart failure patients with primary prophylactic implantable cardioverter defibrillator indication. Europace. 2013 Jun;15(6):820-6. doi: 10.1093/europace/eus430. Epub 2013 Jan 16. PMID: 23325044.