SVT with RBBB
Supraventricular tachycardia with RBBB pattern
SVT with RBBB (supraventricular tachycardia with right bundle branch block) pattern as evidenced by the slurred S wave in lead I and aVL and rSR’ pattern in V1. The right bundle conduction is slower during tachycardia and hence right bundle aberrancy is more likely to occur than left bundle aberrancy. It could also be a pre-existing right bundle branch block. In this case the person had Ebstein’s anomaly of tricuspid valve. Ebstein’s anomaly can be associated with RBBB pattern or polyphasic QRS complexes. They can also have right sided accessory pathways which can predispose to atrioventricular reentrant tachycardia.
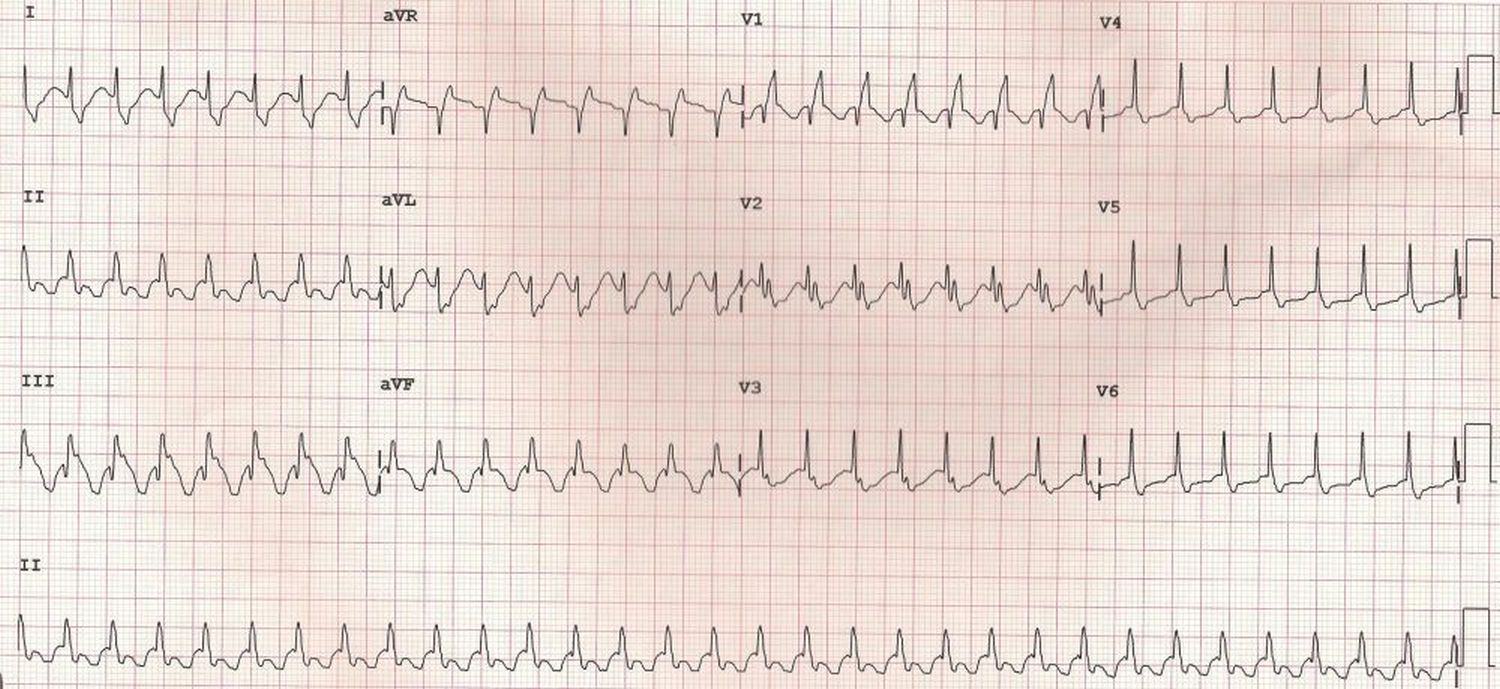
Supraventricular tachycardia with aberrant conduction can be mistaken for ventricular tachycardia due to the wide QRS complex. But a typical right bundle branch block pattern in multiple leads as seen in this case of SVT with RBBB is unlikely in ventricular tachycardia.
12 lead ECG is useful in differentiating SVT with RBBB (or other form of aberrancy) from ventricular tachycardia [1]. But it may be difficult to differentiate in case of fast tachycardias with rate above 190/min. Presence of AV dissociation, if visible on the ECG would point towards ventricular tachycardia.
It is always better to consider a wide QRS tachycardia as ventricular tachycardia until proved otherwise as 80% of wide QRS tachycardias are likely to of ventricular origin [2]. This approach would avoid potential delays and dangers due to delayed diagnosis of a life threatening ventricular tachycardia.
References
- Drew BJ, Scheinman MM. ECG criteria to distinguish between aberrantly conducted supraventricular tachycardia and ventricular tachycardia: practical aspects for the immediate care setting. Pacing Clin Electrophysiol. 1995 Dec;18(12 Pt 1):2194-208.
- Levy S. Differentiating SVT from VT–a personal viewpoint. Eur Heart J. 1994 Apr;15 Suppl A:31-8.

