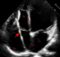
Echocardiography in pulmonary embolism
Echocardiography in pulmonary embolism
Echocardiography in pulmonary embolism is useful in several ways. Visualization of thrombi within the right heart or pulmonary arteries would be the most direct way of diagnosing acute pulmonary embolism by echocardiography. Mobile thrombi in the right heart (Taenia cordis) detected during echocardiography also carries a poor prognosis with higher association with right ventricular dysfunction and mortality. In general, the chance of detection of mobile right heart thrombi in acute pulmonary embolism is about four percent, though up to eighteen percent have been detected in certain intensive care settings. Trans esophageal echo can detect thrombi in central pulmonary arteries as well. Hence it may be a useful investigation when patient is too unstable to be shifted for computerized tomographic pulmonary angiography [1,2].
Other group of echocardiographic findings in acute pulmonary embolism are features of right ventricular overload due to sudden rise in pulmonary arterial pressure and right ventricular dysfunction. Tricuspid regurgitation jet velocity is useful to calculate the right ventricular systolic pressure by the Bernoulli equation (P = 4V2). Main pulmonary artery, right ventricle, right atrium and inferior vena cava can be seen to be dilated in acute pulmonary embolism. Right ventricular dilatation manifests as an increased RV-LV diameter ratio (RV: right ventricle; LV: left ventricle). Relative sparing of right ventricular apex with hypokinesia of right ventricular free wall (McConnell sign) [3] is considered to have a high positive predictive value, though it may not be seen in many cases. A Doppler echocardiographic pattern known as 60/60 sign [4] may also be present. In this case, pulmonary flow acceleration time is less than 60 milliseconds and tricuspid regurgitant jet gradient is less than 60 mm Hg (but more than 30 mm Hg). Tricuspid annular plane systolic excursion (TAPSE) measured by M-Mode echocardiography is also a useful measure of right ventricular systolic function.
Echocardiographic demonstration of right to left shunt across a patent foramen ovale would suggest the possibility of occurrence of paradoxical systemic embolism and thereby connote a higher potential for mortality.
Echocardiography is also useful in differential diagnosis by demonstrating an alternate diagnosis like massive pericardial effusion with cardiac tamponade or aortic dissection. It may be noted that if severe right ventricular hypertrophy and very high tricuspid regurgitation jet gradients are seen, it is likely to be a pre-existing severe pulmonary hypertension as in chronic thromboembolic pulmonary hypertension rather than acute pulmonary embolism. But a person with chronic thromboembolic pulmonary hypertension can also develop acute worsening due to a fresh bout of embolism.
References
- Torbicki A, Galie` N, Covezzoli A, Rossi E, De Rosa M, Goldhaber SZ. Right heart thrombi in pulmonary embolism: results from the International Cooperative Pulmonary Embolism Registry. J Am Coll Cardiol 2003;41(12):2245 – 2251.
- Casazza F, Bongarzoni A, Centonze F, Morpurgo M. Prevalence and prognostic significance of right-sided cardiac mobile thrombi in acute massive pulmonary embolism. Am J Cardiol 1997;79(10):1433 – 1435.
- McConnell MV et al. Regional right ventricular dysfunction detected by echocardiography in acute pulmonary embolism. Am J Cardiol. 1996; 78: 469-473.
- Kurzyna M, Torbicki A, Pruszczyk P, Burakowska B, Fijałkowska A, Kober J, Oniszh K, Kuca P, Tomkowski W, Burakowski J, Wawrzyńska L. Disturbed right ventricular ejection pattern as a new Doppler echocardiographic sign of acute pulmonary embolism. Am J Cardiol. 2002 Sep 1;90(5):507-11.