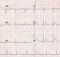
Postural orthostatic tachycardia syndrome
Postural orthostatic tachycardia syndrome
Postural orthostatic tachycardia syndrome (POTS) is characterized by orthostatic tachycardia in the absence of orthostatic hypotension. Criteria for diagnosis of POTS are as follows: 1. Heart rate increase ≥30 beats per minute from supine to standing (5-30 min) 2. Symptoms get worse with standing and better on lying down 3. Symptoms lasting ≥6 months 4. Absence of other overt cause of orthostatic symptoms or tachycardia like active bleeding, acute dehydration and medications [1]. As children have higher orthostatic tachycardia, a cut off of ≥40 beats per minute within 5 minutes of head up tilt has been suggested in young children [2]. An orthostatic heart rate ≥130bpm for ages 13 years and younger or ≥120bpm for ages 14 years and older has also been suggested as an additional criteria.
Both cardiac and non cardiac symptoms can occur in POTS. Cardiac symptoms include rapid palpitations, light headedness, chest discomfort and dyspnea. Non-cardiac symptoms could be mental clouding, headache, nausea, tremulousness, blurred vision, poor sleep, exercise intolerance and fatigue [3]. Fatigue resulting from activities of daily living such as bathing or household work can cause significant limitation of functional capacity.
Large majority of patients are females in the age group 13-50 years [4]. Light headedness was found to vary in them during the menstrual cycle and may be related to changes in estrogen levels. It was more during periods and less during follicular phase. They also reported an increase in estrogen related gynecologic disease [5].
Clinical examination may show features of mitral valve prolapse, though significant mitral regurgitation is rare. Dependent acrocyanosis is a striking physical finding which occurs in 40-50% of patients. A dark red-blue discoloration of legs which are cold to touch can be seen [1].
Two important phenotypes of POTS are the neuropathic POTS and central hyperadrenergic POTS [1]. Partial sympathetic denervation, especially of the legs with less norepinephrine release in the lower extremities has been documented in some patients with neuropathic POTS [6]. Excessive sympathetic discharge may be the underlying mechanism in central hyperadrenergic POTS. They often have extremely high levels of upright plasma norepinephrine. These patients may benefit from central sympatholytics like methyldopa and clonidine. Peripheral beta adrenergic blockers may also be useful in these patients [3]. Some patients with POTS present with episodic flushing and have co-existent mast cell activation as evidenced by increase in urinary methylhistamine [7].
Pheochromocytoma can be considered in the differential diagnosis of POTS because of paroxysmal palpitation. But they are more likely to have symptoms in the supine position and have high plasma norepinephrine levels. Plasma or urine levels of metanephrines have about 98% sensitivity for detecting pheochromocytomas [8]. Holter monitoring may be useful in excluding paroxysmal arrhythmia in case of paroxysmal palpitation. Sometimes the symptoms of POTS may be mistaken for anxiety disorder and panic disorder. Neurally mediated syncope or vasovagal syncope can have symptoms similar to POTS, particularly in the immediate pre-syncopal phase [9].
References
- Raj SR. The Postural Tachycardia Syndrome (POTS): pathophysiology, diagnosis & management. Indian Pacing Electrophysiol J. 2006 Apr 1;6(2):84-99.
- Singer W, Sletten DM, Opfer-Gehrking TL, Brands CK, Fischer PR, Low PA. Postural tachycardia in children and adolescents: what is abnormal? J Pediatr. 2012 Feb;160(2):222-6.
- Raj SR. Postural tachycardia syndrome (POTS). Circulation. 2013 Jun 11;127(23):2336-42.
- Garland EM, Raj SR, Black BK, Harris PA, Robertson D. The hemodynamic and neurohumoral phenotype of postural tachycardia syndrome. Neurology. 2007 Aug 21;69(8):790-8.
- Peggs KJ, Nguyen H, Enayat D, Keller NR, Al-Hendy A, Raj SR. Gynecologic disorders and menstrual cycle lightheadedness in postural tachycardia syndrome. Int J Gynaecol Obstet. 2012 Sep;118(3):242-6.
- Jacob G, Costa F, Shannon JR, Robertson RM, Wathen M, Stein M, Biaggioni I, Ertl A, Black B, Robertson D. The neuropathic postural tachycardia syndrome. N Engl J Med. 2000 Oct 5;343(14):1008-14.
- Shibao C, Arzubiaga C, Roberts LJ 2nd, Raj S, Black B, Harris P, Biaggioni I. Hyperadrenergic postural tachycardia syndrome in mast cell activation disorders. Hypertension. 2005 Mar;45(3):385-90.
- Manger WM, Eisenhofer G. Pheochromocytoma: diagnosis and management update. Curr Hypertens Rep. 2004 Dec;6(6):477-84.
- Bryarly M, Phillips LT, Fu Q, Vernino S, Levine BD. Postural Orthostatic Tachycardia Syndrome: JACC Focus Seminar. J Am Coll Cardiol. 2019 Mar 19;73(10):1207-1228.