Prosthetic valve degeneration and stent creep
Prosthetic valve degeneration and stent creep
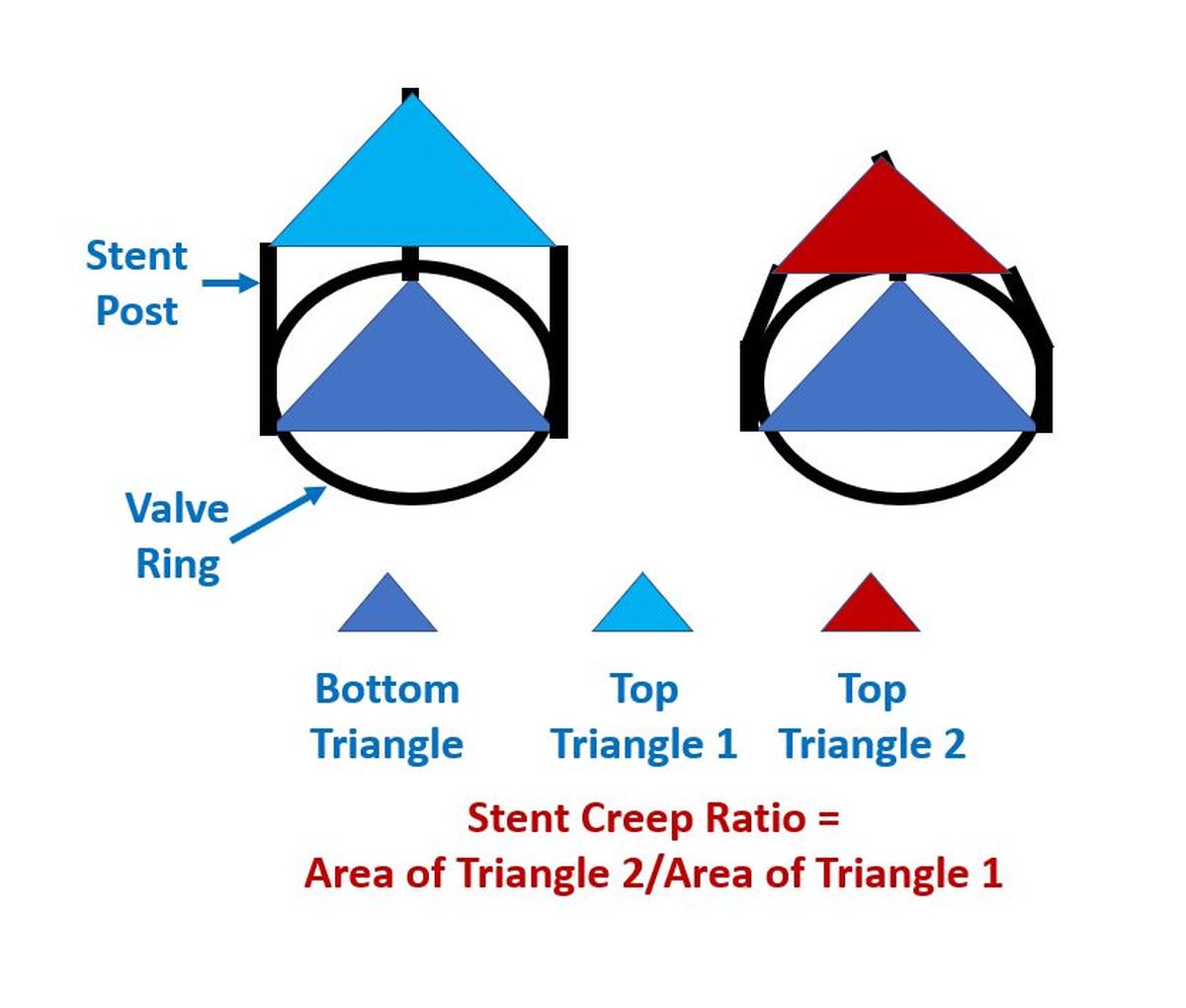
Prosthetic valve degeneration and stent creep: “Stent Creep” seen in some types of bioprosthesis is due to inward bending of the stent struts [1]. It may not be obvious on 2-D echocardiographic imaging, but increases the transvalvular gradient as measured by Doppler echocardiography. Stent creep tends to increase with time after implantation [2]. It was due to an ultrastructural deformity of polypropylene used in the valve stent [3]. This was noted in explanted Hancock bioprosthesis which led to the development of newer stent materials resistant to such deformity.
Valve-in-valve transcatheter aortic valve implantation has been used to treat bioprosthetic failure due to stent creep [4]. They reported three cases, of which two had Carpentier Edwards Perimount prosthesis while one had Mitroflow. Authors suggested that valve oversizing could be the reason for the permanent inward deflection of the stent posts.
Mechanical valve malfunction
Mechanical valve malfunction could be due to ball degeneration, ball variance, strut fracture, thrombus or pannus. Pannus is the growth of fibrous tissue into the valve structure resulting in increase of transvalvular gradient.
References
- Schoen FJ, Schulman LJ, Cohn LH. Quantitative anatomic analysis of “stent creep” of explanted Hancock standard porcine bioprostheses used for cardiac valve replacement. Am J Cardiol. 1985 Jul 1;56(1):110-4.
- Akiyama K, Sawatani O, Imamura E, Endo M, Hashimoto A, Koyanagi H. Clinical study of “stent creep” in porcine bioprosthesis. Nihon Geka Gakkai Zasshi. 1988 May;89(5):747-51.
- Valente M, Bortolotti U, Thiene G, Arbustini E, Milano A, Mazzucco A, Gallucci V. Post bending of the polypropylene flexible stent in mitral Hancock bioprostheses. Eur J Cardiothorac Surg. 1987;1(3):134-8.
- Attia R, Papalexopoulou N, Hancock J, Young C, Thomas M, Bapat V. Successful treatment of failing biological prosthesis because of “Stent creep” with valve-in-valve transcatheter aortic valve implantation. Catheter Cardiovasc Interv. 2015 Aug;86(2):E119-25.
- Kuan-Chih Huang, Wei-Hsian Yin , Yung-Tsai Lee, Tien-Ping Tsao, Kuo-Chen Lee, Ming-Chon Hsiung, Jeng Wei. Quantification of Stent Creep by Three-Dimensional Transesophageal Echocardiography in Patients Undergoing Transcatheter Aortic Valve-in-Valve Implantation for Failed Bioprostheses. Acta Cardiol Sin. 2019 Jul;35(4):380-386.

