Thrombus aspiration during primary angioplasty
Thrombus aspiration during primary angioplasty
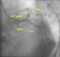
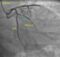
Thrombus aspiration during primary angioplasty: Primary angioplasty is currently the best method for treating persons with acute ST elevation myocardial infarction presenting during the window period. Embolisation of atherothrombotic material during primary angioplasty often leads to obstruction of microvasculature and the well known ‘slow flow phenomenon’. Various methods have been evaluated for reducing the chance for microvascular obstruction during primary angioplasty. Currently one of the popular methods is to aspirate the thrombus within the lumen of the artery and remove it. Thrombus aspiration produces better reperfusion and clinical outcomes. Aspiration is often considered when there is a visible thrombus on angiography. The device is introduced soon after the occlusive lesion is crossed by the guide wire. The aspiration catheter is introduced into the thrombus containing region under continuous aspiration. The whole unit is then withdrawn over the guidewire and the aspirated thrombus taken out. Care should be taken to avoid spillage of the thrombus into major proximal branches which can have catastrophic results. Negative suction is maintained while withdrawing the catheter. Care should be taken to prevent undue advancement of the guide catheter which may occur during this withdrawal process.
One initial study which showed benefit with thrombus aspiration was published in NEJM [1]. But later studies (TASTE and TOTAL) did not favour the use of routine thrombus aspiration [2,3]. So the initial enthusiasm for thrombus aspirated faded out. But it is still being used in selected cases with high thrombus loads.
References
- Tone Svilaas, Pieter J Vlaar, Iwan C van der Horst, Gilles F H Diercks, Bart J G L de Smet, Ad F M van den Heuvel, Rutger L Anthonio, Gillian A Jessurun, Eng-Shiong Tan, Albert J H Suurmeijer, Felix Zijlstra. Thrombus aspiration during primary percutaneous coronary intervention. N Engl J Med. 2008 Feb 7;358(6):557-67.
- Ole Fröbert, Bo Lagerqvist, Göran K Olivecrona, Elmir Omerovic, Thorarinn Gudnason, Michael Maeng, Mikael Aasa, Oskar Angerås, Fredrik Calais, Mikael Danielewicz, David Erlinge, Lars Hellsten, Ulf Jensen, Agneta C Johansson, Amra Kåregren, Johan Nilsson, Lotta Robertson, Lennart Sandhall, Iwar Sjögren, Ollie Ostlund, Jan Harnek, Stefan K James, TASTE Trial. Thrombus aspiration during ST-segment elevation myocardial infarction. N Engl J Med. 2013 Oct 24;369(17):1587-97.
- Sanjit S Jolly 1, John A Cairns 2, Salim Yusuf 3, Michael J Rokoss 3, Peggy Gao, Brandi Meeks, Sasko Kedev, Goran Stankovic, Raul Moreno, Anthony Gershlick, Saqib Chowdhary, Shahar Lavi, Kari Niemela, Ivo Bernat, Warren J Cantor, Asim N Cheema, Philippe Gabriel Steg, Robert C Welsh, Tej Sheth, Olivier F Bertrand, Alvaro Avezum, Ravinay Bhindi, Madhu K Natarajan, David Horak, Raymond C M Leung, Saleem Kassam, Sunil V Rao, Magdi El-Omar, Shamir R Mehta, James L Velianou, Samir Pancholy, Vladimír Džavík, TOTAL Investigators. Outcomes after thrombus aspiration for ST elevation myocardial infarction: 1-year follow-up of the prospective randomised TOTAL trial. Lancet. 2016 Jan 9;387(10014):127-35.