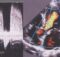
Estimation of PCWP from E/E’ on Tissue Doppler Imaging
Estimation of PCWP from E/E’ on Tissue Doppler Imaging
Conventionally, pulmonary capillary wedge pressure (PCWP) is measured using a catheter in the pulmonary artery. Pulmonary artery diastolic pressure measured by a Swan Ganz balloon floatation catheter at bedside is often taken as the surrogate of PCWP. Ideal method of bedside measurement is balloon occlusion of a pulmonary artery branch to get the distal pressure. But it cannot be done on a continuous basis as it will compromise flow to the territory and vascular complications can ensue. True PCWP, as the name implies, is obtained after wedging an end hole catheter with no side holes (Cournand catheter), during right heart catheterization.
Nagueh formula can be used for calculation of PCWP from the Doppler derived mitral E/E’ ratio [1]. PCWP is usually equal to the left atrial pressure and hence the left ventricular filling pressure. E’ (Ea) has been considered as a preload independent index of left ventricular relaxation. Nagueh formula uses mitral E velocity during early diastolic flow corrected for the influence of left ventricular relaxation (E/E’ ratio) to estimate the mean PCWP [1].
Nagueh formula: PCWP = 1.24 [E/E’] + 1.9
Ea was taken from the lateral mitral annulus in the pioneering study of Nagueh SF et al. 60 patients had invasive measurement of PCWP and simultaneous Doppler echocardiography [1].
Comparison of pulmonary arterial diastolic pressure by an implantable device known as CardioMEMS™ with left atrial pressure measured from transthoracic echocardiography in 17 patients has been reported [2]. Left atrial pressure was assessed by tissue Doppler imaging using Nagueh formula. The study was in patients with congestive heart failure and showed direct linear correlation between pulmonary artery diastolic pressure and simultaneously measured left ventricular filling pressure by echocardiography. They had averaged septal and lateral mitral annular velocities for calculation of PCWP using Nagueh formula.
Sugimoto T et al studied 165 patients with almost equal number of heart failure with preserved ejection fraction (HFpEF) and heart failure with reduced ejection fraction (HFrEF) [3]. In their study, PCWP had the strongest correlation with E/A ratio (ratio peak early mitral inflow velocity E to peak late diastolic mitral inflow velocity during atrial contraction A) in both groups. This was followed by left atrial diameter and E/E’. Receiver operating characteristic (ROC) analysis showed that the combination of abnormal E′ ≤8 and elevated E/A had high diagnostic accuracy compared with E/E′ in both HFpEF and HFrEF. Cutoff values of E/A was 1.81 in HFpEF and 1.16 in the HFrEF group for predicting mean PCWP >18 mmHg.
In sharp contrast with these reports, Mullens W et al did not find a correlation between mitral E/Ea and PCWP in their prospective study of advanced decompensated heart failure in New Heart Association class III-IV with left ventricular ejection fraction ≤30% [4]. These patients underwent simultaneous echocardiography and hemodynamic evaluation on admission and after 48 hours of intensive medical therapy. The lack of correlation was more in those with larger left ventricular volumes, more impaired cardiac reflexes and in the presence of cardiac resynchronization therapy. The sensitivity and specificity for mitral E/Ea ratio 15 to identify a PCWP 18 mm Hg were 66% and 50%, respectively. But several letters to the editor were published including one by Nagueh SF on behalf of the ASE and EAE Diastology Writing Group which pointed out several limitations in the methodology [5].
References
- Nagueh SF, Middleton KJ, Kopelen HA, Zoghbi WA, Quiñones MA. Doppler tissue imaging: a noninvasive technique for evaluation of left ventricular relaxation and estimation of filling pressures. J Am Coll Cardiol. 1997 Nov 15;30(6):1527-33.
- Tolia S, Khan Z, Gholkar G, Zughaib M. Validating Left Ventricular Filling Pressure Measurements in Patients with Congestive Heart Failure: CardioMEMS™ Pulmonary Arterial Diastolic Pressure versus Left Atrial Pressure Measurement by Transthoracic Echocardiography. Cardiol Res Pract. 2018 Jul 15;2018:8568356.
- Sugimoto T, Dohi K, Tanabe M, Watanabe K, Sugiura E, Nakamori S, Yamada T, Onishi K, Nakamura M, Nobori T, Ito M. Echocardiographic estimation of pulmonary capillary wedge pressure using the combination of diastolic annular and mitral inflow velocities. J Echocardiogr. 2013 Mar;11(1):1-8.
- Mullens W, Borowski AG, Curtin RJ, Thomas JD, Tang WH. Tissue Doppler imaging in the estimation of intracardiac filling pressure in decompensated patients with advanced systolic heart failure. Circulation. 2009 Jan 6;119(1):62-70.
- Nagueh SF; ASE and EAE Diastology Writing Group. Letter by Nagueh et al regarding article, “Tissue Doppler imaging in the estimation of intracardiac filling pressure in decompensated patients with advanced systolic heart failure”. Circulation. 2009 Aug 18;120(7):e44.