Grossly dilated inferior vena cava (IVC)
Grossly dilated inferior vena cava (IVC)
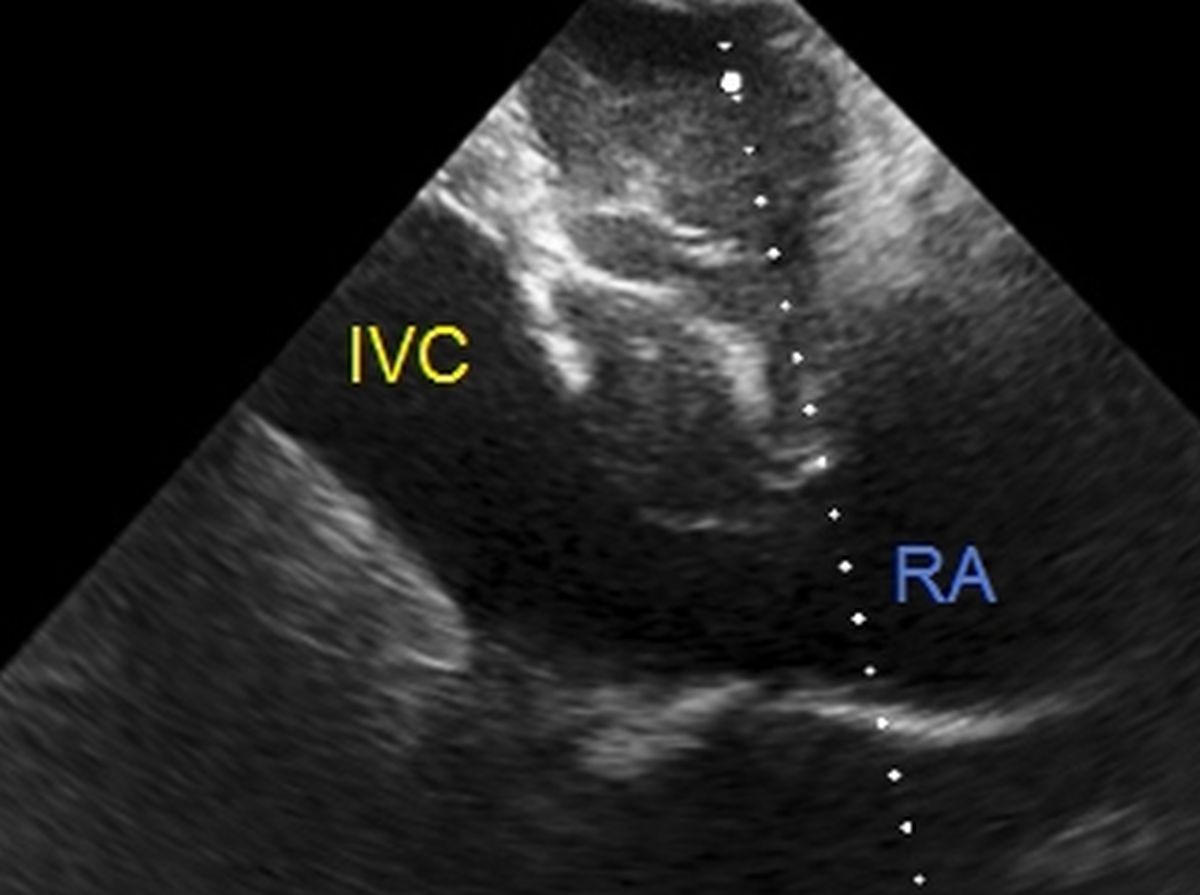 Grossly dilated inferior vena cava (IVC): Subcostal view with a tilt can image the inferior vena cava (IVC) draining into the right atrium (RA). Here the IVC is grossly dilated, with a diameter of 40 mm, indicating severe right heart failure. When IVC is dilated very much it is customary to add 20 mm Hg to the observed tricuspid regurgitation gradient while estimating the right ventricular systolic pressure. Dilated IVC without an inspiratory collapse is known as IVC plethora. IVC can be dilated in constrictive pericarditis, without associated enlargement of right heart chambers. Zig-zag movement of sonodense particles in a dilated IVC in constrictive pericarditis has been called the traffic jam sign.
Grossly dilated inferior vena cava (IVC): Subcostal view with a tilt can image the inferior vena cava (IVC) draining into the right atrium (RA). Here the IVC is grossly dilated, with a diameter of 40 mm, indicating severe right heart failure. When IVC is dilated very much it is customary to add 20 mm Hg to the observed tricuspid regurgitation gradient while estimating the right ventricular systolic pressure. Dilated IVC without an inspiratory collapse is known as IVC plethora. IVC can be dilated in constrictive pericarditis, without associated enlargement of right heart chambers. Zig-zag movement of sonodense particles in a dilated IVC in constrictive pericarditis has been called the traffic jam sign.
IVC measurement is often used to guide fluid resuscitation in the acute care setting instead of the conventional measurement of central venous pressure by a catheter. This is convenient being non-invasive and easily available in modern day emergency departments and critical care/intensive care units equipped with a point of care ultrasound machine. In a person presenting with hypotension, if IVC is collapsed, a fluid bolus can be given fast, often with rapid recovery.
Post surgical patients will need different approach to imaging IVC as the epigastric region may be covered with surgical dressing. In these cases, imaging through the liver from right infra axillary region is very useful, though it is often a bit tricky and needs experience to get a good view of the IVC. Luboch M and colleagues evaluated the inferior vena cava/aorta index measured with the transducer placed in the anterior median line and right anterior axillary line [1]. They concluded that measurements from both sites can be used interchangeably in determining the body fluid status.
Reference
- Luboch M, Łoś M, Szmygel Ł, Kosiak W. Sonographic assessment of the inferior vena cava/aorta index measured with the transducer placed in the anterior median line and right anterior axillary line – a comparison. J Ultrason. 2014 Sep;14(58):280-6.
