Patent ductus arteriosus
Patent ductus arteriosus
Ductus arteriosus normally closes by 72 hours after birth. The structure becomes fibrotic later and remains as the ligamentum arteriosum. Endothelium of mature ductus responds to oxygen which acts as the stimulus of constriction as it receives oxygenated blood from the lungs. Premature ductus does not respond to oxygen that well. Patent ductus arteriosus is much more common in the premature infant than the mature infant. The higher the prematurity, the higher the chance of having a patent ductus arteriosus (PDA). PDA can occur as part of the congenital rubella syndrome.
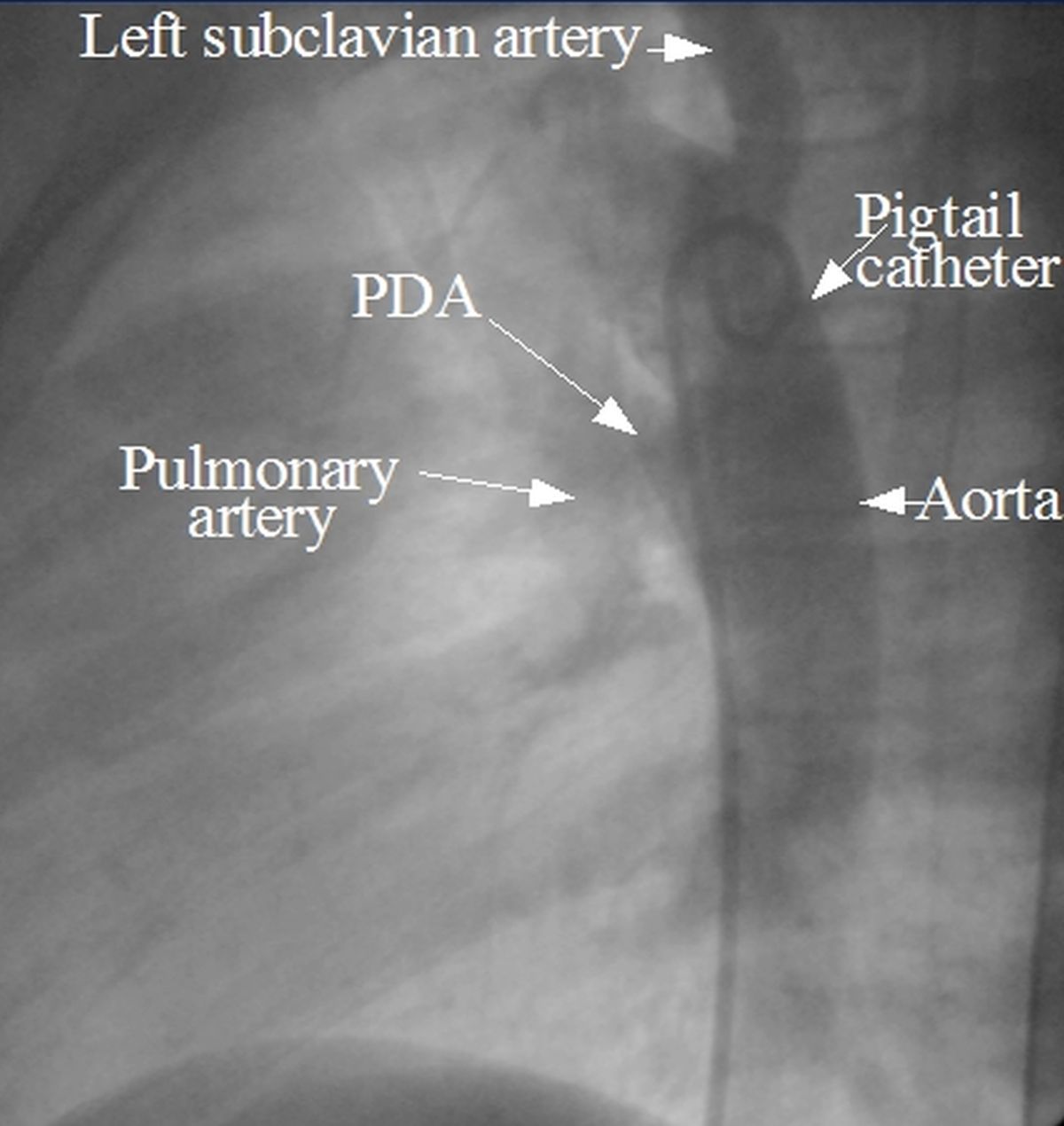
Patent ductus arteriosus demonstrated by an aortogram. The aortogram was obtained after injecting radiocontrast dye into the aorta using a catheter. Dye is seen entering the pulmonary artery through the PDA from the descending aorta.
Patent ductus arteriosus with left to right shunt increases pulmonary blood flow, pulmonary venous return and dilatation of left atrium, left ventricle and aorta. When there is a large flow, pulmonary arteries are dilated and long standing cases develop severe pulmonary hypertension with flow reversal (Eisenmenger reaction). The patent ductus arteriosus connects to the aorta distal to the origin of left subclavian. Hence reversal of shunt produces desaturation mostly in the lower part of the body, leading to differential cyanosis and clubbing. Upper body receives saturated blood from the aorta prior to the right to left shunt and has no cyanosis.
Clinical findings in PDA
Pulse is high volume in PDA because the flow from aorta into the low resistance pulmonary circuit acts as an aortic runoff. Increased load to the left ventricle produces cardiomegaly with left ventricular type of forceful apex beat. The classical murmur in PDA is a continuous murmur which peaks around the second sound. It is also known as train in tunnel murmur and Gibson’s murmur as best heard below the left clavicle (Gibson’s area). The train in tunnel character is imparted by the addition of multiple vascular clicks known as eddy sounds, due to the highly turbulent flow through the ductus. A continuous thrill is often associated. The diastolic component of the murmur becomes inaudible with the development of pulmonary hypertension and the murmur may be confined to systole (Atypical PDA). But signs of pulmonary hypertension like palpable pulsations in second left intercostal space with dullness on percussion and a loud pulmonary component of second heart sound (P2) may be evident then.
Chest X-ray in PDA
PDA with large left to right shunt will show pulmonary plethora, left ventricular type of cardiomegaly, prominent aortic shadow, enlarged main pulmonary artery and branch pulmonary arteries.
X-ray appearance of calcification of patent ductus arteriosus: Typical appearance of calcification of patent ductus arteriosus in an X-ray chest PA view is inverted Y shaped. Inverted Y shape is a combined appearance of calcification of the aortic arch extending down to the pulmonary artery and patent ductus arteriosus.