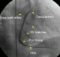
Carotid artery stenting for acute internal carotid occlusion
Carotid artery stenting for acute internal carotid occlusion
Internal carotid occlusion is known to produce a massive stroke with significant morbidity and mortality. The results of intravenous thrombolysis may not be good with only about seventeen percent achieving good clinical outcome and a mortality as high as fifty five percent. Panagiotis Papanagiotou, Christian Roth, Silke Walter, Stefanie Behnke, Iris Q Grunwald, Julio Viera, Maria Politi, Heiko Körner, Panagiotis Kostopoulos, Anton Haass, Klaus Fassbender and Wolfgang Reith evaluated the role of stenting in acute stroke due to atherosclerotic extracranial internal carotid artery occlusion [1]. They could treat twenty two patients within six hours of onset of stroke symptoms. Some of these patients had additional intracranial lesions in the internal carotid or middle cerebral artery. These were treated with special devices for the purpose or a combination of mechanical recanalization and intra arterial thrombolysis. Recanalization was assessed by immediate post procedure angiography and neurological status was evaluated before treatment and minimum follow up upto three months using the National Institutes of Health Stroke Scale and the modified Rankin Scale. Successful recanalization of extracranial internal carotid artery was achieved in ninety five percent of patients and sixty one percent achieved TIMI (Thrombolysis In Myocardial Infarction) 2/3 flow. Mortality was 13.6 percent at three months. The authors concluded that carotid artery stenting for acute atherosclerotic occlusion of the extracranial portion of the internal carotid artery with a severe stroke is feasible, safe and useful if done within first six hours of onset of symptoms. Forty one percent of their patients had a modified Rankin Scale of two or less at three months.
Reference
- Panagiotis Papanagiotou, Christian Roth, Silke Walter, Stefanie Behnke, Iris Q Grunwald, Julio Viera, Maria Politi, Heiko Körner, Panagiotis Kostopoulos, Anton Haass, Klaus Fassbender, Wolfgang Reith. Carotid artery stenting in acute stroke. J Am Coll Cardiol. 2011 Nov 29;58(23):2363-9.