Proarrhythmia
Proarrhythmia
Proarrhythmia can be defined as the aggravation of an existing arrhythmia or the development of a new arrhythmia secondary to an antiarrhythmic drug [1]. This usually occurs at a drug dose which is considered to be below the toxic level. Proarrhythmia could be an acceleration of a tachycardia or causing of a clinically significant bradyarrhythmia.
Types of Proarrhythmia: Polymorphic tachycardia or torsades, monomorphic ventricular tachycardia, atrial flutter with 1:1 conduction, alteration of thresholds of devices inducing arrhythmia.
Genetic component is involved in most cases of proarrhythmia. Sometimes genetic factors may manifests only when one pathway is blocked by disease and another is affected genetically. This situation occurs in the setting of renal failure.
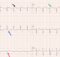
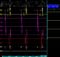
Pathophysiology of torsades – usually seen in a structurally normal heart. EAD (early afterdepolarization) and DAD (delayed afterdepolarization) are important mechanisms. EAD occurs in phases 2 or 3. DAD is due to early phase 4 re-entry. Basic reason for all these is prolongation of refractoriness.
EAD is seen in conditions like low pacing rates, hypokalemia. DAD is seen in conditions with intra cellular calcium overload – catecholamines, hypoxia and cardiac glycosides.
Goal of antiarrhythmic therapy is two fold: 1) conversion of unidirectional block to bidirectional block. 2) prolongation of myocardial refractoriness. (1) is achieved by affecting the sodium channels and depolarization while (2) is achieved by affecting the repolarization.
When repolarization is prolonged EADs can occur triggering a reentrant tachycardia. This occurs with class IA drugs and does not occur in class IB and C.
Monomorphic reentrant tachycardia can occur in the setting of myocardial infarction. Class IC drug can depress conduction to such an extent that recovery of some regions facilitate re-entry. This does not occur with type IA drugs. Class IC can cause incessant re-entrant monomorphic VT. For this reason, monomorphic VT occurs in the setting of a structurally abnormal heart while torsades occur in the setting of a structurally normal heart.
Multiple drug withdrawals have occurred in various countries due to concerns of proarrhythmia [2]. Testing for QT interval prolongation is now mandatory during drug development.
Conventionally, sotalol is started in hospital, for monitoring efficacy and proarrhythmia. Outpatient initiation with the help of implanted cardiac implantable electronic devices (CIED) for monitoring has been studied [3]. These were patients with paroxysmal or persistent atrial fibrillation eligible for rhythm control strategy. After a process of shared decision making, outpatient initiation of sotalol was done, with regular clinical encounters and assessment utilizing remote monitoring of CIED. Cardiac rhythm and QTc intervals were monitored. There were 105 patients in the study cohort, with mean CHA2DS2-VASc score of 3.26. Of these, 26 patients had permanent pacemakers, 10 had dual chamber implantable cardioverter defibrillators and 69 had implantable loop recorders. Over a follow up period of 23 ± 15 months, sotalol was continued in 77 who maintained sinus rhythm. It was discontinued in 28 because of inefficacy or adverse effects. There were no adverse effects related to prolongation of QTc, torsades or morality during the study period.
Comprehensive in vitro Proarrhythmia Assay initiative (CiPA, https://cipaproject.org ) project for cardiac safety includes both in vitro analysis and in silico reconstructions of cellular cardiac electrophysiologic activity [4]. This may help in predicting proarrhythmia in drugs under development.
Reference
- Naccarelli GV, Wolbrette DL, Luck JC. Proarrhythmia. Med Clin North Am. 2001 Mar;85(2):503-26, xii.
- Turner JR, Rodriguez I, Mantovani E, Gintant G, Kowey PR, Klotzbaugh RJ, Prasad K, Sager PT, Stockbridge N, Strnadova C; Cardiac Safety Research Consortium. Drug-induced Proarrhythmia and Torsade de Pointes: A Primer for Students and Practitioners of Medicine and Pharmacy. J Clin Pharmacol. 2018 Aug;58(8):997-1012.
- Mascarenhas DAN, Mudumbi PC, Kantharia BK. Outpatient Initiation of Sotalol in Patients with Atrial Fibrillation: Utility of Cardiac Implantable Electronic Devices for Therapy Monitoring. Am J Cardiovasc Drugs. 2021 Jul 22:1–8.
- Mathie A, Veale EL, Golluscio A, Holden RG, Walsh Y. Pharmacological Approaches to Studying Potassium Channels. Handb Exp Pharmacol. 2021 Jul 1.